The Final Chapter
Glaucoma and the eye removal
In late January of 2015, after only a few months of seeing well, Peanut’s vision seemed to get worse suddenly. We went to our local GP for an eye pressure check. The pressure was sky high indicating glaucoma. We next made an emergency visit to yet another eye specialist — Dr. Enry Garcia with VCA Aurora. Garcia ordered a pressure curve and it confirmed glaucoma. The silicone oil leakage from the retina surgery caused a blockage in the drainage system. By the time we noticed the change in vision, the optic nerve was permanently damaged. Less than ten months after the retina reattachment surgery at Eye Care for Animals, Peanut had an attached retina but was completely blind nevertheless.
Garcia did not explain to us at the time that treating glaucoma with drops would only delay having to remove the eye because of pressure spikes and the pain they caused. So we kept up with 7-8 drops a day of various medications from February of 2015 through September of 2016. Despite those drops we always wondered if Peanut was experiencing bad headaches due to pressure spikes. Suddenly on October 6, 2016, Peanut cried out in pain with the slightest touch of his head (a gentle kiss) and cried out again and again even when a hand came near his head. We rushed him to our GP and asked for a pressure check. His pressure was again sky high. Drops every two hours seemed to reduce the pain.
After an examination the next day, Dr. Garcia told us that Peanut’s glaucoma now required a change in tactic. He gave us two options. We could try an injection to clear the drainage system and reset the whole process (drops to control pressure, etc.). Alternatively, we could try an injection that would kill the cells that cause drainage thereby eliminating the need for future drops. The first option didn’t appeal to us because it was only delaying the inevitable return of pressure spikes. We didn’t want Peanut to experience pain from pressure spikes ever again. The second option supposedly had an 80% success rate. We knew the silicone oil in Peanut’s eye could cause problems with that second option; it was a variable that made any prediction of success impossible. Plus since the retina reattachment was supposed to have a 90% success rate and turned out so disastrously, we didn’t feel confident about another experimental surgery with a supposed high rate of success. So we told our doctor that we wanted to pursue a third option that seemed the most logical and would guarantee 100% success. We told him we wanted Peanut’s eye removed. He had no vision anyway.
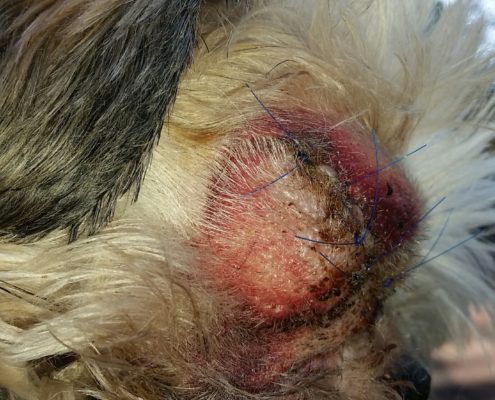
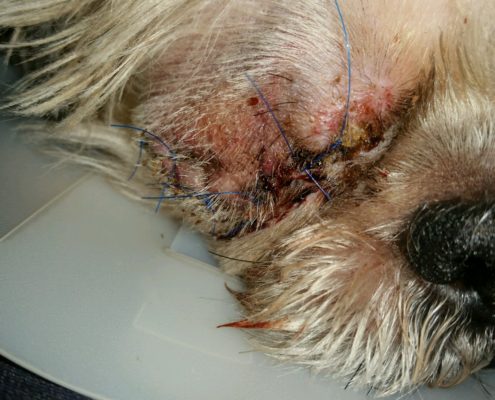
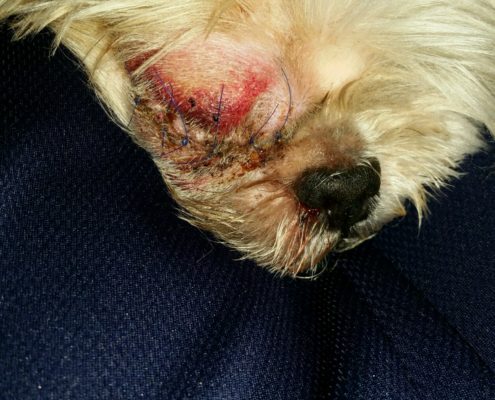
Whereas any GP can perform an eye removal, we opted to have Dr. Garcia handle the surgery. Although an abscess developed that required antibiotics, we are happy with our decision. Within a week of having his eye removed, Peanut was like a new dog. He was more spunky, sassy, alert and energetic than he had been since before the retina reattachment surgery. He has a new lease on life now. More than anything we regret not removing the eye in the first place after the diagnosis of a detached retina. We would have had a spunkier, sassier and happier dog two years earlier than now. We could have put the many thousands of dollars spent on surgeries, daily medications, office visits and pressure checks toward a family vacation with our dogs. And we would have sparred Peanut and ourselves years of tremendous pain, suffering and sadness. Given that a dog’s primary senses are smell and hearing and that dogs don’t need to look in the mirror, eye removal is a smart way to go.
Dr. Garcia did not recommend a prosthetic or implant as part of Peanut’s eye removal surgery. We have heard that some specialists DO recommend this sort of cosmetic procedure. In our opinion, a prosthetic is a waste of money. Your pet won’t need to worry about its appearance in order to get a job or attract the opposite sex. An experienced groomer can work wonders with the appearance of a one-eyed or no-eyed pet. After a while, you won’t even notice what’s missing; you’ll just see your pet. Furthermore, artificial implants of any kind can lead to complications. We remember hearing a customer in the Eye Care for Animals lobby expressing deep regret for following the practice’s recommendation for a prosthetic. The appearance of the prosthetic was terrible and there had been a serious infection.
ADDENDUM: In 2016, we received a postcard mailer announcing that Dr. Kimberly Hsu is now performing retina reattachment surgery (replacing Sisler) at Eye Care for Animals in Naperville, IL. She was a resident studying under Sisler. We believe that she learned and practiced on Peanut and we were never told that was going to happen. Although she has denied it, we still believe she was actively involved in the April 2014 surgery on Peanut that led to the terrible story told on this website. It is a fact that Dr. Hsu has much less experience in performing this experimental surgery than other retina surgeons across the U.S. and Canada. It is also a fact that she did her residency with Eye Care for Animals and trained under Steve Sisler. We have been told by a surgeon who performs retina reattachment on humans that the best veterinary eye surgeons train on humans and do their residencies at universities and colleges (as opposed to for profit vet specialty clinics). In our opinion, no one should subject their pet to a retina reattachment surgery. If, after reading everything we’ve posted here, a pet owner still wants to go the route of having retina surgery performed, look to the most experienced surgeon. Also remember that when something goes wrong with a retina surgery, your local GP and your local eye specialist will not have any idea what do to about it. You’ll need to travel back to the practice where the surgery was performed.